Scars
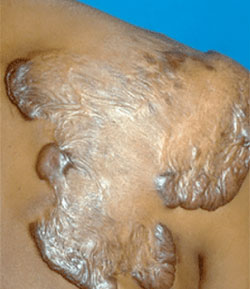
Different types of scars require different treatment. Many scars can be treated if they make you feel uncomfortable around others, cause pain, or restrict your movement.
Scars: Diagnosis and treatment
Why should a dermatologist diagnose what type of scar you have?
While it may seem obvious that you have a scar, it’s important to have a dermatologist examine it before it’s treated.
Scars are complex. To treat you safely and effectively, it’s important for the person treating you to know about your health and the type of scar you have.
Different types of scars require different treatment. Your age and how long you’ve had the scar may also affect the types of treatment that will work best for you.
A board-certified dermatologist has the training and experience required to tell you:
- What type(s) of scar you have
- If a scar is likely to fade with time
- When to treat the scar to get the best results
- What treatment is recommended
It’s also important to have a dermatologist examine your scar because sometimes skin cancer can look like a scar. If you see a scar on your skin and don’t remember injuring your skin, immediately make an appointment to see a board-certified dermatologist.
Another good reason to see a dermatologist before having a scar treated is to make sure it’s still just a scar. Sometimes, skin cancer develops in a scar. You can reduce this risk by always wearing sunscreen when clothing won’t cover your scar. To give you the protection you need, always use a broad-spectrum sunscreen with SPF 30 or higher.
You also want to avoid tanning beds, which increase your risk of developing skin cancer.
How do dermatologists prevent and treat scars?
The treatments described on this page apply mainly to raised scars and keloids. You’ll find information about treating other types of scars on these pages:
If you have a raised scar or keloid, your dermatologist may recommend one or more of the following treatments.
Pressure therapy: Applying pressure to a wound while it’s healing can:
- Reduce (or prevent) a scar, especially while a burn heals
- Prevent a keloid if your skin tends to form this type of scar
- Prevent a keloid from returning after it’s surgically removed
To apply pressure, a patient wears a pressure dressing, which may be an elastic bandage, stocking, or earring.
Some patients find the pressure dressing uncomfortable and stop wearing it too soon. To get results, however, you may have to wear the pressure dressing for as long as one year. You may also need to get a new pressure garment every 6 to 8 weeks.
If you have a wound on your face, pressure therapy is not a treatment option.
Silicone gel (sheet or ointment): Used since 1982, silicone can:
- Treat a raised scar by reducing its size, hardness, redness, swelling, itch, or stiffness
- Prevent a raised scar, especially after surgery
- Prevent a scar from developing after surgery to remove the scar
Studies show that the silicone gel sheets appear to work better than the silicone ointment.
The gel sheets are thin and self-adhesive. You use them after the wound closes. To get results, you must wear a gel sheet every day, often for months. Having this in the same spot every day can cause side effects. The skin can breakdown. Some people develop a rash.
If side effects occur, tell your dermatologist. You may need to stop wearing the sheeting and use another treatment.
Polyurethane dressing: This is a moist, flexible pad. You wear it to:
- Reduce scarring after surgery
- Treat a raised scar by reducing the color, hardness, and size
When worn for six weeks after surgery, it may prevent a raised scar. Studies have shown that patients who wear a moist dressing with a pressure garment get better results than patients who use one or the other.
Lasers and other light treatments: This is becoming the go-to treatment for all types of scars because these treatments can:
- Prevent raised scars and keloids
- Reduce the appearance of existing raised scars and keloids
- Decrease scarring after surgery
- Treat some depressed acne scars
- Lessen the color of the scar, such as redness
- Increase a person’s ability to move when a scar limits movement
- Reduce pain, itch, hardness, and swelling
Studies show that laser therapy or pulse-dye light can give patients impressive results. In the skilled hands of a board-certified dermatologist, these offer patients a safe treatment option with few side effects.
To give patients the best results from laser or light treatments, a dermatologist may also inject a medication, such as corticosteroids or 5-FU, into the scar.
For more information on laser treatment for scars, go to 10 things to know before having laser treatment for your scar.
Corticosteroid injections: Widely used to treat raised scars and keloids, dermatologists inject a corticosteroid directly into the scar to:
- Reduce the size of a raised scar or keloid
- Ease symptoms of itch and pain
Studies show that it can reduce the size of a scar by 50% or more. In some cases, it can look like the scar is completely gone.
To get results, most people need more than one treatment.
Possible side effects include the scar returns, thinning skin, and dark spots where you had the injection.
To reduce possible side effects, you may receive another scar treatment, such as an injection of 5-FU or treatment with a pulsed-dye laser.
5-FU or bleomycin injections: Your dermatologist may inject one of these medications directly into the scar to:
- Reduce (or completely flatten) a raised scar or keloid
- Ease symptoms of itch and pain
Possible side effects include redness, swelling, thinning skin, or dark spots where you received the injection.
To reduce these possible side effects, a patient often receives another scar treatment, such as a corticosteroid injection or pulsed-dye laser therapy.
Cryosurgery: This treatment freezes the scar, which slowly destroys the scar tissue. Dermatologists have used this treatment for years to:
- Reduce the size of raised scar or keloid
- Reduce pain, itch, hardness, and discoloration
After one treatment, the freezing can reduce the size of a scar by 50% or more.
To reduce the size of a scar even more, a patient may also receive an injection of a medication, such as corticosteroid or 5-FU.
Scar surgery: During this treatment, a dermatologic surgeon cuts out the scar. In the hands of board-certified dermatologic surgeon, scar surgery can:
- Reduce the size of a keloid
- Increase your ability to move if a scar limits movement
While surgery can be effective, it is usually only an option when other treatment fails. A scar can return after it’s removed. To reduce the risk of this happening with a keloid, the surgeon often leaves the border of the keloid in place.
To improve results, another treatment, such as injections of a corticosteroid, is often given to patients who have scar surgery.
Radiation: Studies show that radiation therapy can:
- Reduce raised scars and keloids when other treatments fail
- Relieve the itch and discomfort that sometimes occurs in raised scars and keloids
- Lessen the risk of a scar returning after scar surgery
Very few patients receive radiation therapy because there is a concern that it can cause cancer years later. Other possible side effects include dark spots, itch, redness, and swelling.
Other treatments for scars: You’ll find non-prescription scar treatments that contain ingredients such as onion extract, vitamin A, and vitamin E. Research on how well these work is limited. Before using one of these, the AAD recommends that you speak with a board-certified dermatologist.
Images
Image 1: Used with permission of the American Academy of Dermatology National Library of Dermatologic Teaching Slides.
References:
American Academy of Dermatology. “Scar treatment can help improve patients’ quality of life.” News release issued July 28, 2016. Last accessed November 14, 2017.
Tziotzios C, Profyris C, et al. “Cutaneous scarring: Pathophysiology, molecular mechanisms, and scar reduction therapeutics Part II. Strategies to reduce scar formation after dermatologic procedures.” J Am Acad Dermatol. 2012;66:13-24.
Zurada JM, Kriegel D, et al. “Topical treatments for hypertrophic scars.” J Am Acad Dermatol. 2006;55:1024-31.
© 2026 American Academy of Dermatology. All rights reserved. Reproduction or republication strictly prohibited without prior written permission. Use of these materials is subject to the legal notice and terms of use located at https://www.aad.org/about/legal

